Cholesterol has become one of the most misunderstood substances in the body. It is often spoken about as if it were a toxin that must be lowered at all costs, yet it is one of the most essential molecules for life. Every cell membrane depends on it. Hormones depend on it. The brain, which is largely made of fat, relies heavily on it. Without cholesterol, there is no structure, no signaling, and no stability.
So how did something so fundamental become the focus of fear?
The confusion begins with how cholesterol is measured and interpreted. Clinical tests report total cholesterol, LDL, HDL, and triglycerides. These numbers are then placed into categories of risk, often without context. When LDL is elevated, it is labeled as dangerous. When total cholesterol is high, it is treated as a problem to be reduced. What is often missed is that these numbers do not tell us why cholesterol is elevated or what the body is trying to do with it.
Cholesterol does not move through the body on its own. It is transported in lipoproteins, which are essentially delivery vehicles. LDL is one of those vehicles. It is not inherently harmful. It is part of a system that moves fats, repairs tissues, and responds to damage. When LDL is elevated, it often reflects increased transport activity. The body is moving material where it is needed.
This is where the interpretation begins to shift.
When there is damage in the body, whether from oxidative stress, inflammation, or tissue breakdown, the body responds. Cholesterol is sent to those areas as part of the repair process. It helps stabilize cell membranes and supports regeneration. If the underlying stress continues, the transport continues. Over time, this can lead to accumulation. The accumulation is then labeled as the problem, when in reality it is the response.
This is why simply lowering cholesterol does not address the root issue.
The medical approach has largely focused on reducing cholesterol levels through medication. Drugs designed to lower cholesterol can be effective at changing the numbers on a lab report. However, they do not resolve the underlying terrain that led to the increased transport in the first place. In many cases, they interfere with essential processes in the body. Cholesterol is required for hormone production, nerve function, and cellular communication. When its production or transport is artificially suppressed, other systems can be affected.
People often report fatigue, muscle weakness, cognitive changes, and reduced resilience when these pathways are disrupted. These are not isolated side effects. They are signals that the body is being pushed away from its natural balance.
This creates a deeper problem.
When the focus remains on lowering a number, the original cause continues. The body may still be dealing with inflammation, poor lipid processing, digestive inefficiency, or mineral imbalance. The signal remains, but the response is suppressed. Over time, this can lead to further dysfunction rather than resolution.
From a terrain perspective, cholesterol is not the enemy. It is a participant in a larger system.
To understand what is happening, we need to look beyond the lab report and observe how the blood is behaving in real time.
In live blood analysis, cholesterol itself is not seen directly. What we see are patterns that reflect how fats and proteins are being handled in the body.
One of the most common findings is rouleau formation. Red blood cells stack together like coins, indicating thicker plasma and reduced flow. This often correlates with poor fat and protein metabolism and suggests that the internal environment is becoming congested.
Another marker is the presence of lipid particles in the plasma. These appear as floating droplets or a cloudy background. This reflects fats that are not being properly processed or cleared. It is a visual indication that transport and movement are not functioning efficiently.
Fibrin may also be present. These are fine strands or web-like structures in the plasma that indicate inflammatory signaling and reduced circulation. When flow is compromised, fibrin tends to increase, further contributing to stagnation.
Protein dysregulation can also be observed. Red blood cells may appear misshapen, often taking on a tear drop or lemon shape. This reflects issues with protein breakdown and membrane integrity, both of which are closely tied to how fats are integrated and used in the body.
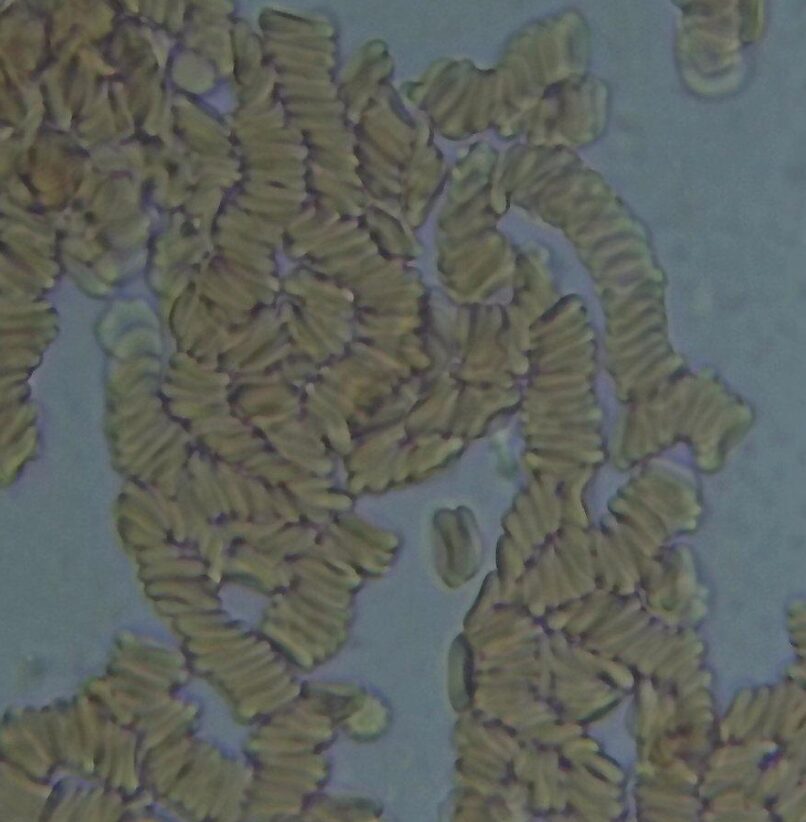
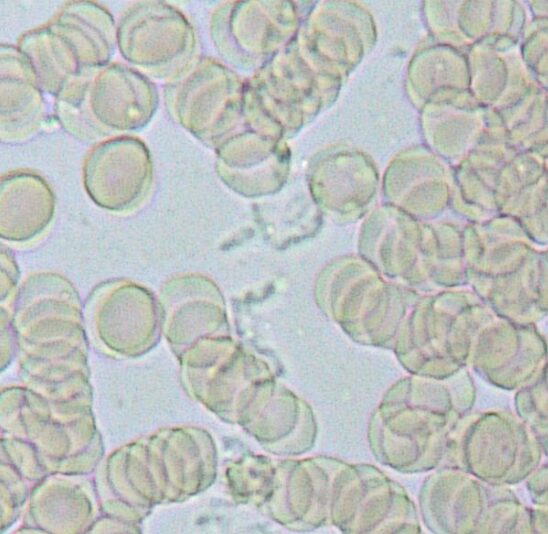
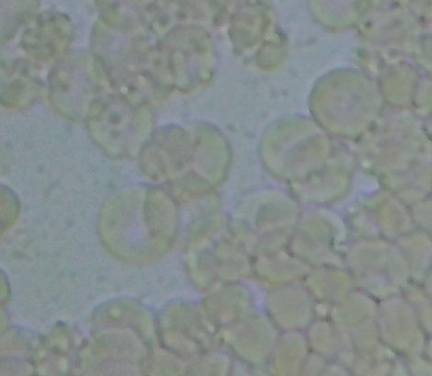
Taken together, these markers tell a story.
They show a system where movement has slowed, where materials are not being properly processed, and where the body is working to compensate. In this context, elevated cholesterol in a lab test begins to make sense. It is not a random elevation. It is part of a coordinated response to imbalance.
This is why the statement that LDL is “bad” does not hold up under closer examination. LDL is a carrier. When it is elevated, it is often because the body is attempting to move and repair. The real question is not how to eliminate LDL, but why the body is calling on it more heavily.
When we shift the focus from suppression to understanding, the approach changes.
Instead of asking how to lower cholesterol, we ask how to restore flow. We look at digestion, because fats must be properly broken down and emulsified. We look at the microbial environment, because microbes influence how fats are processed and transported. We look at mineral balance, because it affects how oxygen and nutrients move through the blood. We look at inflammation, because it drives the need for repair.
This is a more complete picture.
Cholesterol is not the starting point of disease. It is part of the body’s attempt to maintain stability in the face of disruption. When we recognize this, we stop fighting the response and begin to understand the cause.
From there, the path forward becomes clearer.
What Cholesterol Medications Actually Do, and Why That Matters
When cholesterol becomes the focus, medication is often introduced with the goal of lowering measurable levels. These drugs are effective at shifting numbers on a lab report, but it is important to understand how they achieve that change and what else is affected in the process.
The most commonly prescribed medications are statins. They work by blocking a key enzyme in the liver that is involved in the production pathway of cholesterol. When this pathway is interrupted, the liver reduces its output, and circulating levels of LDL tend to decrease.
However, this pathway is not dedicated to cholesterol alone. It is part of a broader system responsible for producing several compounds the body relies on daily. One of these is CoQ10, which plays a central role in cellular energy production. When the pathway is suppressed, CoQ10 levels can decline, and this can show up as reduced energy, muscle fatigue, or a general sense of depletion.
This same pathway is also tied to the production of compounds that support hormonal balance. When it is altered, the body may have to adjust how it regulates stress, sleep, and overall resilience. These changes are not always immediate, but they can become more noticeable over time.
There are also medications that work in different ways. Some reduce how much cholesterol is absorbed through the digestive tract, while others influence how it is transported in the bloodstream. Although their mechanisms differ, the end goal remains the same, which is to reduce circulating levels.
The challenge with this approach is that it focuses on the outcome rather than the conditions that led to that outcome. When a number is lowered without addressing the underlying processes that created it, the body continues to operate under the same pressures. The visible marker changes, but the internal environment may not.
Another layer to consider is how these interventions affect the body as an interconnected system. When one pathway is altered, others adjust in response. Changes in how fats are processed can influence digestion, which in turn affects the microbial environment of the gut. That microbial environment plays a role in how fats are metabolized and circulated. What appears to be a targeted intervention often has wider effects.
This is why some people experience changes that extend beyond what they expected. These are not random reactions. They reflect the body adapting to a shift in one of its core pathways.
There are situations where medication is used to manage immediate concerns, and that context matters. The issue arises when the focus remains on suppression alone, without exploring how to restore the systems that regulate balance over time.
When we step back and look at the bigger picture, the question becomes less about how to lower a number and more about how to support the body so that the number no longer needs to be elevated.
Restoring Balance Naturally: Working With the System
At this point, the focus shifts.
If cholesterol reflects movement, repair, and transport, then the goal is not to suppress it. The goal is to restore the conditions where movement is efficient, repair is complete, and nothing accumulates unnecessarily. This requires looking at how fats are handled from the very beginning, not just how they appear on a lab report.
This means returning to digestion, food structure, microbial activity, and the daily patterns that determine how the body processes and moves what it takes in.
As I was looking deeper into this, I came across a newer approach being discussed around arterial health. It involved a compound called cyclodextrin. It is being used in some circles to support the movement of cholesterol within the body.
Rather than focusing on the product itself, I wanted to understand what it was actually doing.
Cyclodextrins are formed when microbes act on starch and reorganize it into a ring-shaped structure. This structure has the ability to bind to fat-like compounds and keep them suspended in a fluid environment. In simple terms, it can hold onto lipids and help keep them moving rather than allowing them to accumulate.
That immediately raised a more important question.
If this function can exist in an isolated compound, then how does the body normally perform this role, and how can we support that process through food, herbs, fermentation, and the way we prepare what we eat?
Because in a living system, this should not depend on a single substance. It should be part of a coordinated process.
From that point, the approach becomes much clearer. Instead of trying to replicate the compound, we begin to rebuild the system that performs the same function.
A Simple Natural Protocol
This is not about forcing change. It is about restoring the conditions that allow the body to move, organize, and use fats properly.
This is also not an overnight fix. The patterns that lead to stagnation develop over time, and they resolve the same way. Slowly, consistently, and with the right inputs. When this is done properly, it becomes very effective because it is not overriding the body. It is training it. It is instructing it. It is giving it the means to return to its own processes of regulation and repair.
Step One: Prepare the System Before Food Enters
Begin the day, and ideally each main meal, with warm water, lemon or lime, and a small pinch of sea salt. A small amount of fermented liquid can be added if available.
This is not just a habit. It is a signal that prepares the entire digestive system.
This simple step stimulates stomach acid, enzymes, and most importantly bile. Bile is what allows fats to be broken down into smaller droplets so they can move through a watery environment rather than separating and becoming stagnant. Without this step, fats are far more likely to be poorly handled from the beginning.
Sip this slowly and allow a few minutes before eating. That pause gives the body time to respond.
You can also include bitter greens or herbs such as dandelion, arugula, or fresh garden herbs with meals to further support this process. Bitters are one of the most direct ways to stimulate bile and keep fats moving.
Step Two: Create a Binding Matrix
Include soaked chia seeds or flax seeds daily.
Add one tablespoon to water and allow them to sit for at least 20 minutes, or overnight for a thicker gel. This can be taken on its own or added to meals.
When hydrated, these seeds form a gel that surrounds fats and keeps them organized during digestion. Instead of fats moving freely and unpredictably, they are held within a structure that supports proper breakdown and transport.
This mimics, in a natural way, the function of holding lipids in a suspended and manageable form.
Step Three: Bring in Microbial Transformation
Include fermented vegetables, fermented grains such as soaked or lightly soured oats, or fermented root preparations each day.
Even a few spoonfuls with meals is enough to begin shifting the internal environment.
These foods introduce active microbial communities that continue the digestive process. They influence how fats are transformed, how bile is recycled, and how compounds are processed before they enter circulation.
This is a key step. Without microbial involvement, the system remains incomplete.
One of the reasons cyclodextrins exist at all is because of microbial activity, particularly from species within the Bacillus family. These microbes act on starch and reorganize it into those ring-shaped structures that can bind and carry lipids.
That matters because it shows us something important.
The ability to bind and move fats is not something foreign to the body. It is something that emerges from microbial interaction with food.
When you include fermented foods and lightly fermented starches, you are engaging similar microbial pathways. You are not producing isolated cyclodextrins in a controlled way, but you are supporting the same type of transformation, where microbes interact with carbohydrates and influence how fats are handled in the system.
You can also prepare simple fermented starches at home by soaking oats, yuca, or potatoes in water for 24 to 48 hours and allowing a light fermentation to occur. This brings microbial activity directly into the foods you are eating and supports the same processes that underlie how compounds are bound, transformed, and moved.
This is where the system begins to come alive.
Step Four: Use Structured Starches
Include cooked and cooled potatoes, rice, yuca, or plantain regularly.
Cook as usual, then allow them to cool fully before eating. They can be eaten cold or gently reheated, but the cooling step is what changes their structure.
This creates resistant starch, which feeds microbial populations that regulate fat metabolism and influence how lipids are handled beyond digestion.
This step connects directly to the earlier point about microbial transformation. It provides the fuel those microbes need to do their work.
Step Five: Combine Fats Within a Living Meal
Build meals that include a cooled starch, fresh herbs or greens, a stable fat such as butter, tallow, or coconut, fermented vegetables, and a spoon of soaked chia or flax.
The goal is structure and coordination.
Fats should not be eaten in isolation. When they are combined with fiber, microbes, and properly prepared starches, they are bound, emulsified, and guided through digestion and into circulation in a controlled way.
Use whole, stable fats rather than highly processed oils. The body handles intact fats very differently than fragmented ones.
A simple meal prepared this way creates the environment where fats are carried, transformed, and moved rather than left to accumulate.
What to Expect Over Time
This approach works through consistency rather than intensity.
As these steps are repeated daily, digestion improves, bile flow becomes more efficient, microbial balance shifts, and the body becomes better at handling and transporting fats.
In live blood, this may be reflected as less rouleau formation, clearer plasma, fewer visible lipid particles, and improved overall movement.
This is the body relearning how to regulate itself, using the inputs it has been given.




